As a prepper, you probably already know how to address problems like natural disasters, social unrest or a long-term power outage. But do you know how to help someone experiencing carbon monoxide poisoning? (h/t to PreppersWill.com)
What causes carbon monoxide poisoning?
Carbon monoxide (CO) is an odorless and colorless gas. CO is found in combustion or exhaust fumes from the following sources:
- Car engines
- Car mufflers
- Charcoal grills
- Fireplaces
- Heaters
- Portable generators
- Space heaters
You're exposed to small amounts of CO every day, but inhaling too much of the gas will cause carbon monoxide poisoning. CO can reach dangerous levels when combustion fumes are trapped in poorly ventilated or enclosed spaces, like your garage. When you inhale these fumes, CO may build up in your bloodstream, causing severe tissue damage.
Carbon monoxide is flammable. With enough oxygen and intense heat, CO will quickly oxidize to form carbon dioxide. This is the mechanism that causes “backdraft.” A poorly ventilated fire inside a closed structure immediately consumes the available oxygen.
CO poisoning is severe and may be life-threatening. Call 911 immediately if you are or someone else is experiencing symptoms of CO poisoning. (Related: Air pollution can also happen INDOORS – here’s how to spot the worst offenders.)
Symptoms of carbon monoxide poisoning
During normal respiration, oxygen-rich air enters your lungs. The oxygen travels through the walls of your alveoli and combines chemically with hemoglobin in the blood, forming oxyhemoglobin.
The blood travels through the pulmonary vein to your heart as it pumps blood to the body’s arterial system. Once the blood arrives near a cell that needs more oxygen, the oxygen-hemoglobin bond is broken and oxygen migrates through the cell wall.
At the same time, the carbon dioxide produced by cell metabolism goes through the cell wall and combines with the hemoglobin. The final product, hemoglobin carbamate, travels through your circulatory system until it returns to the lungs.
Once the carbon dioxide-hemoglobin bond is broken as it reaches the alveoli, the carbon dioxide passes into your lungs and is expelled as you exhale.
While this chemical process is fairly straightforward, you may experience negative side effects once CO enters your lungs.
The National Fire Protection Association (NFPA) Fire Protection Handbook warns that carbon monoxide combines 210 times more readily with hemoglobin than oxygen. However, the produced compound, carboxyhemoglobin, is carried all over your body. As carboxyhemoglobin arrives at an oxygen-deficient cell, no exchange of gasses takes place.
This makes the cell retain the carbon dioxide, making it anoxic before the cell dies. This is why the mechanism of injury of CO poisoning is called hypoxia, or oxygen deficiency, which causes asphyxiation.
Common symptoms of CO poisoning include:
- Confusion
- Difficulty breathing
- Dizziness
- Dull headache
- Nausea
- Vomiting
- Weakness
If you inhale large amounts of CO, your body will start to replace the oxygen in your blood with CO. This can make you lose consciousness or even cause death. If you suspect that you've been exposed to CO, seek medical attention even if you don't experience any of the symptoms above.
Experts warn that CO is harmful to pregnant women, with research suggesting that carboxyhemoglobin levels in the baby are at least twice that of the mother. Other people vulnerable to CO include those with chronic lung problems and children, who have a relatively high respiratory rate and small volume of blood.
Treating carbon monoxide poisoning
If you see someone suffering from CO poisoning, wear a self-contained breathing apparatus (SCBA) to protect yourself then help them evacuate the area immediately.
Note that field treatment for CO poisoning aims to address acute problems and offer supportive therapy. Once you're in a safe place, try to elevate the victim’s head to reduce cerebral edema or swelling of the brain.
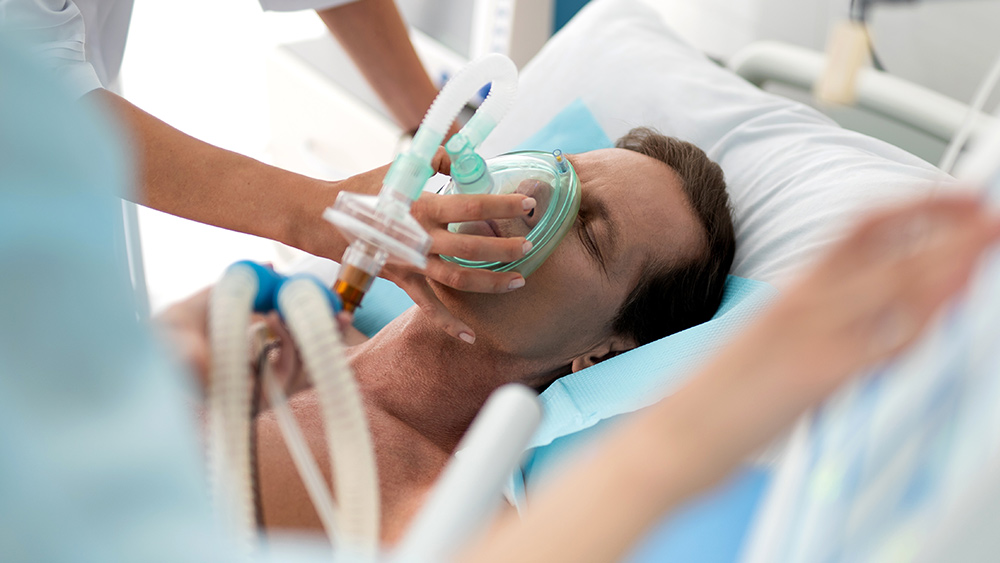
When helping a conscious patient, administer 100 percent oxygen via a mask with an attached oxygen reservoir. Encourage hyperventilation in the patient, loosen any tight clothing and keep them warm until help arrives to efficiently utilize the remaining unattached hemoglobin in their body.
Once the patient is stable, check them for signs of smoke inhalation. Treat burns as needed and check for singed facial and nasal hairs. If the patient makes noisy breathing sounds, they may have inhaled smoke from the fire and suffered thermal burns in their airway. Check the patient's exhaled gasses for soot. If you notice any of these signs, they may be suffering from bronchospasm, pulmonary edema or laryngeal edema.
A patient with edema requires endotracheal intubation to prevent airway obstruction. If possible, contact emergency medical responders with advanced life support capabilities. Don't give the patient narcotic analgesics if they have inhaled smoke or CO because these drugs may have respiratory depressant effects.
When using devices that emit large amounts of CO, ensure that the room you're in has proper ventilation. CO is a silent killer and the best way to treat CO poisoning is to address its symptoms immediately in a survival situation.
Sources include:
Please contact us for more information.