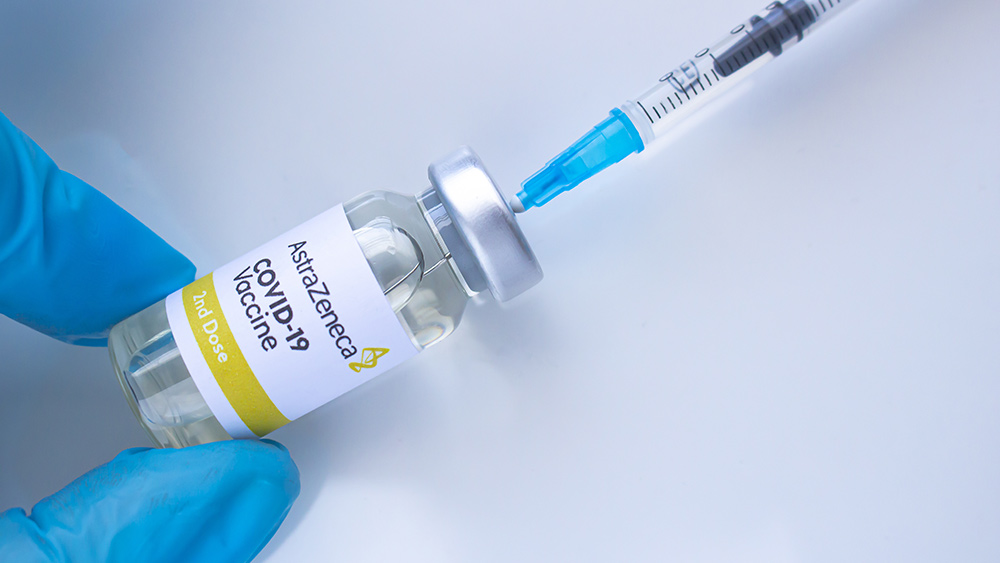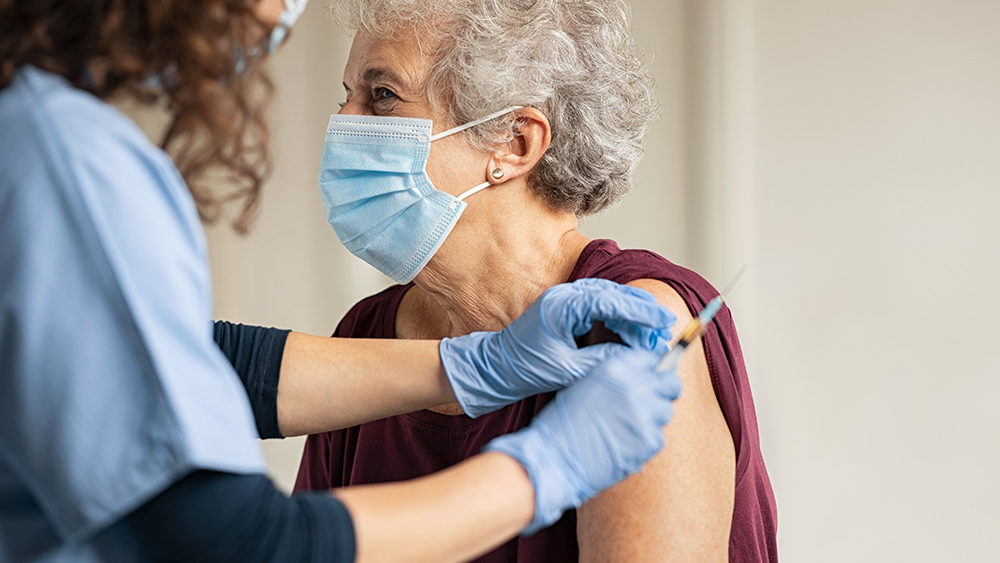
A physician at the Boston Medical Center (BMC) suffered an allergic reaction after receiving the much-talked about Moderna vaccine. The incident, which occurred on Dec. 24, involved Dr. Hossein Sadrzadeh, a geriatric oncologist with a severe allergy to shellfish. Sadrzadeh reported symptoms of anaphylaxis similar to what he experiences with shellfish almost immediately after receiving the Moderna shot.
According to The New York Times, this is the first report of an adverse reaction linked to the Moderna vaccine, which rolled out across the United States a week before the incident. The Food and Drug Administration (FDA) is investigating similar reports of allergic reaction to Pfizer's vaccine, which was distributed a week earlier than Moderna's.
What happened and what may have triggered it
In a statement, BMC spokesman David Kibbe confirmed that Sadrzadeh was inoculated with Moderna's vaccine at 3:30 pm on Christmas Eve. Within minutes of receiving the shot, the doctor, who has serious allergies, had a severe reaction that required him to use his EpiPen -- an auto-injectable device containing epinephrine that's used in emergency situations to treat severe allergic reactions, or anaphylaxis. Sadrzadeh was then taken to the emergency room where he was evaluated, treated, observed and discharged four hours later.
Sadrzadeh later recounted his experience in an interview and likened it to the anaphylactic reaction triggered in him by shellfish. Besides feeling dizzy and faint, he said that his heart rate had spiked to 150 beats per minute and that his tongue had prickled and gone numb. Sadrzadeh also said that his blood pressure plummeted and that his immune system was in revolt. According to a record of his visit to the ER, Sadrzadeh was given several medications, including steroids and Benadryl, to calm his immune reactions to the COVID-19 vaccine. The doctor gave a personal report of his experience to Moderna and a national vaccine safety surveillance system run by the FDA and the CDC.
Moderna's vaccine is one of only two COVID-19 vaccines currently authorized by the FDA for emergency use during the coronavirus pandemic. Since the rollout of the Pfizer-BioNTech vaccine on Dec. 14, healthcare workers have received top priority for immunization. Unlike the vaccines developed for other diseases, these two vaccines are a new type of injectable medication. Called messenger RNA (mRNA) vaccines, they are made with genetic material copied from the coronavirus instead of a weakened or inactivated version of the pathogen.
The goal of mRNA vaccines, according to CDC, is to instruct cells to produce a harmless piece of a viral protein -- in this case, the spike protein that the coronavirus uses to infect cells. This innocuous protein then triggers an immune response and allows the body to build a suitable defense against the COVID-19 virus. This, theoretically, would give whoever receives the vaccine protection against COVID-19 without having to risk getting sick with the viral disease. (Related: Moderna admits that some components of mRNA tech used in vaccines can cause “significant adverse events”.)
However, despite repeated assurances by both Pfizer and Moderna that their vaccines are safe, several experts have raised concerns about a particular ingredient used in mRNA vaccines. Polyethylene glycol (PEG) is a compound derived from petroleum and is used in various industrial products. In the form of tiny spheres, PEG is used to protect the mRNA in Pfizer and Moderna's vaccines and help it penetrate cells. But according to Dr. Peter Marks, the director of the FDA's Center for Biologics Evaluation and Research, this compound may be the culprit behind the anaphylactic reactions associated with the vaccines.
PEG has never been used before in any approved vaccine, mainly because there is no need for it. But there have been reports of certain drugs containing PEG occasionally causing anaphylaxis symptoms, such as rashes, shortness of breath, plummeting blood pressure and palpitations. Experts have also raised the possibility of people previously exposed to the compound having high levels of antibodies against it. This potentially puts them at great risk of a severe allergic reaction should they receive either one of the approved vaccines.
Pfizer's vaccine is also causing allergic reactions
Just days after the distribution of Pfizer's COVID-19 vaccine began in the U.S., reports emerged of recipients suffering multiple allergic reactions. At a press conference held that same week, a total of five cases in more than one state were confirmed by the FDA, two of which occurred in the same hospital in Alaska. According to The New York Times, one of the workers who was rushed to the emergency room developed a rash over her face and torso, experienced shortness of breath and an elevated heart rate -- symptoms similar to what Sadrzadeh later experienced after receiving Moderna's vaccine.
The other recipient, meanwhile, complained of lightheadedness and a scratchy throat and developed eye puffiness 10 minutes after receiving the shot. But unlike the first recipient, who had to spend the night in the intensive care unit, the second recipient recovered quickly and was released within an hour. The FDA immediately issued a warning for Americans who have a history of severe allergic reactions but insisted that the vaccine is still safe. Some experts, however, noted the similarities between the reported allergic reactions and those seen in the United Kingdom.
Britain began administering the Pfizer-BioNTech vaccine on Dec. 8. On the first day of the country's mass vaccination program, two cases of allergic reactions were reported and confirmed, prompting the U.K. medical regulator to issue a public warning for those with a history of serious allergic reactions. While Pfizer and BioNTech reported finding "no serious safety concerns" in late-stage trials of their vaccine, a review of the documents published by the two companies revealed that people with serious allergies were excluded from the trials.
The FDA is currently working with the CDC to investigate the reported adverse reactions. The two agencies and the three companies behind the approved vaccines still maintain that the COVID-19 shots are safe. As of Dec. 31, as many as 10 people in the U.S. have experienced anaphylaxis after receiving shots.
Sources include:
Please contact us for more information.